
Parents of deceased patient also complained of inappropriate medication, communication
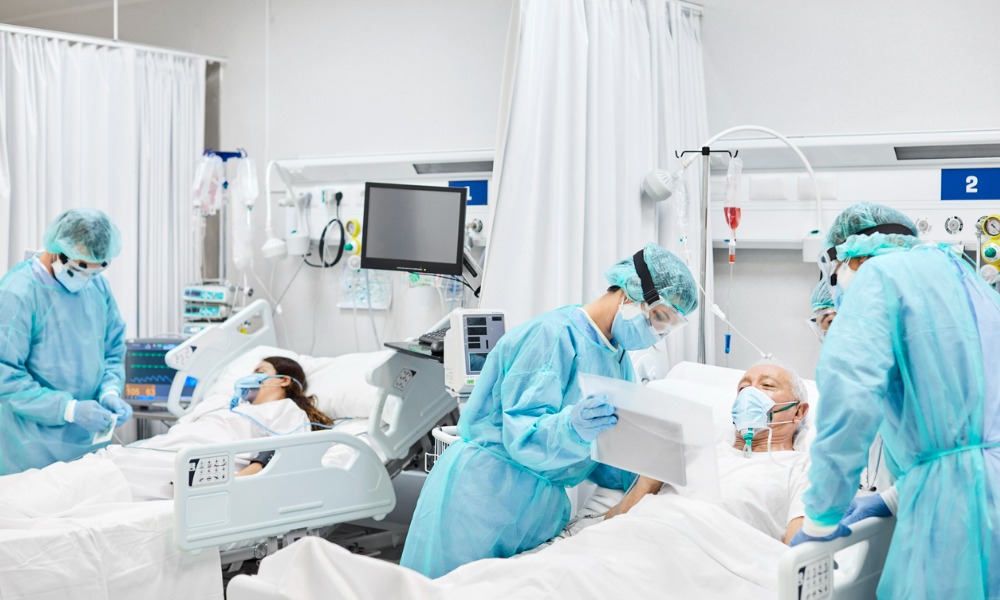
A review board has upheld a committee’s finding that it was unnecessary to call a code blue for a patient already in an intensive care unit (ICU) with respiratory technicians, nursing staff, and an intensivist team at the bedside, actively resuscitating.
The patient’s medical history in Shaikh v. Redstone, 2022 CanLII 90634 (ON HPARB) included developmental delay, seizure disorder, hypothyroidism, and a permanent tracheostomy. She had a gastric feeding tube and could not stand, speak, or communicate, depending on her parents for all activities of daily living.
In February 2021, the patient received admission to Mackenzie Health’s ICU in Vaughn, ON, with a diagnosis of sepsis secondary to pneumonia. The respondent, an internist and critical care specialist, became her attending critical care physician. The patient died the following month.
The applicant, who was the patient’s mother, brought a complaint claiming that the respondent inappropriately prescribed the patient an anticoagulant without the parents’ knowledge or consent and continued ordering and administering this medication until the patient’s death, despite telling the parents that it would be discontinued. The medication allegedly led to excessive bleeding from the patient’s mouth, nose, and vagina.
The respondent also allegedly failed to:
The Inquiries, Complaints and Reports Committee of the College of Physicians and Surgeons of Ontario investigated the complaint and decided to take no further action. However, it noted that it expected physicians to communicate with substitute decision-makers as soon as possible.
The committee found that the patient was treated for pneumonia after her admission to the ICU, that the respondent regularly and frequently communicated with the patient’s parents, that the nursing staff administered pain medication as needed, and that the medical record supported the respondent’s claim that it was inappropriate to call a code blue while the patient still had a pulse. The applicant requested a review.
The Health Professions Appeal and Review Board of Ontario confirmed the committee’s decision under s. 35(1) of Ontario’s Health Professions Procedural Code. The board noted that physicians were expected to communicate with substitute decision-makers as soon as possible.
The board determined that the committee’s investigation was adequate and covered the essential information relevant to arriving at an informed decision on the issues. The parties made no challenge to the investigation’s adequacy and received numerous opportunities to provide information, said the board.
Next, the board decided that the committee’s decision was reasonable. The committee clearly considered the applicant’s concerns, addressed each one, and coherently explained its conclusions. The committee, in tackling each concern, frequently and specifically referred to the contemporaneous medical record to support its conclusions, the board said.
The board held that the committee’s decision was transparent, intelligible, and justified. The decision showed a coherent and rational connection among the relevant facts, the decision’s outcome, and the reasoning process leading to the outcome, the board concluded.